How oxygen and carbon dioxide are transported in the blood
Content:
- Introduction
- Transporting oxygen
- Carrying oxygen
- Foetal haemoglobin
- Transporting carbon dioxide
- The effect of carbon dioxide
The most specialised transport role of the blood is the transport of oxygen from the lungs to the cells of the body by the erythrocytes (red blood cells).
The erythrocytes are also involved in the removal of carbon dioxide from the cells and its transport to the lungs for gaseous exchange.
Transporting oxygen
The erythrocytes are very specialised, with a number of adaptations to their main function of transporting oxygen.
Erythrocytes have a biconcave shape.
This shape has a larger surface area than a simple disc structure or a sphere, increasing the surface area available for diffusion of gases.
It also helps them to pass through narrow capillaries.
In adults, erythrocytes are formed continuously in the red bone marrow.
By the time mature erythrocytes enter the circulation they have lost their nuclei, which maximises the amount of haemoglobin that fits into the cells.
It also limits their life, so they only last for about 120 days in the bloodstream.
Erythrocytes contain haemoglobin, the red pigment that carries oxygen and also gives them their colour.
Haemoglobin is a very large globular conjugated protein made up of four peptide chains, each with an iron-containing haem prosthetic group.
There are about 300 million haemoglobin molecules in each red blood cell and each haemoglobin molecule can bind to four oxygen molecules.
The oxygen binds quite loosely to the haemoglobin forming oxyhaemoglobin.
The reaction is reversible.
You may have miss
Blood vessels, Blood, Tissue Fluid, and Lymph
The need for specialised transport systems in animals
Urine and pregnancy testing
Carrying oxygen
When the erythrocytes enter the capillaries in the lungs, the oxygen levels in the cells are relatively low.
This makes a steep concentration gradient between the inside of the erythrocytes and the air in the alveoli.
Oxygen moves into the erythrocytes and binds with the haemoglobin.
The arrangement of the haemoglobin molecule means that as soon as one oxygen molecule binds to a haem group, the molecule changes shape, making it easier for the next oxygen molecules to bind.
This is known as positive cooperativity.
Because the oxygen is bound to the haemoglobin, the free oxygen concentration in the erythrocyte stays low, so a steep diffusion gradient is maintained until all of the haemoglobin is saturated with oxygen.
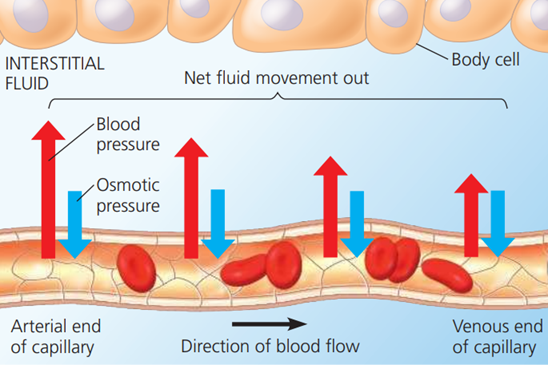
When the blood reaches the body tissues, the situation is reversed.
The concentration of oxygen in the cytoplasm of the body cells is lower than in the erythrocytes.
As a result, oxygen moves out of the erythrocytes down a concentration gradient.
Once the first oxygen molecule is released by the haemoglobin, the molecule again changes shape and it becomes easier to remove the remaining oxygen molecules.
Note:
When you are not very active, only about 25% of the oxygen carried in your erythrocytes is released into the body cells. The rest acts as a reservoir for when the demands of the body increase suddenly.
Foetal haemoglobin
When a foetus is developing in the uterus it is completely dependent on its mother to supply it with oxygen.
Oxygenated blood from the mother runs close to the deoxygenated foetal blood in the placenta.
If the blood of the foetus had the same affinity for oxygen as the blood of the mother, then little or no oxygen would be transferred to the blood of the foetus.
However, foetal haemoglobin has a higher affinity for oxygen than adult haemoglobin.
So, it removes oxygen from the maternal blood as they move past each other.
Transporting carbon dioxide
Carbon dioxide is transported from the tissues to the lungs in three different ways:
- About 5% is carried dissolved in the plasma.
- 10-20% is combined with the amino groups in the polypeptide chains of haemoglobin to form a compound called carbaminohaemoglobin.
- 75-85% is converted into hydrogen carbonate ions in the cytoplasm of the red blood cells.
Most of the carbon dioxide that diffuses into the blood from the cells is transported to the lungs in the form of hydrogen carbonate ions.
Carbon dioxide reacts slowly with water to form carbonic acid.
The carbonic acid then dissociates to form hydrogen ions and hydrogen carbonate ions.
In the blood plasma this reaction happens slowly.
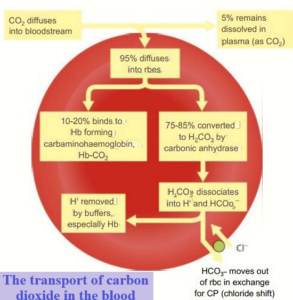
However, in the cytoplasm of the red blood cells there are high levels of the enzyme carbonic anhydrase.
This enzyme catalyses the reversible reaction between carbon dioxide and water to form carbonic acid.
The carbonic acid then dissociates to form hydrogen carbonate ions and hydrogen ions.
The negatively charged hydrogen carbonate ions move out of the erythrocytes into the plasma by diffusion down a concentration gradient and negatively charged chloride ions move into the erythrocytes, which maintains the electrical balance of the cell.
This is known as the chloride shift.
By removing the carbon dioxide and converting it to hydrogen carbonate ions, the erythrocytes maintain a steep concentration gradient for carbon dioxide to diffuse from the respiring tissues into the erythrocytes.
When the blood reaches the lung tissue where there is a relatively low concentration of carbon dioxide, carbonic anhydrase catalyses the reverse reaction, breaking down carbonic acid into carbon dioxide and water.
Hydrogen carbonate ions diffuse back into the erythrocytes and react with hydrogen ions to form more carbonic acid.
When this is broken down by carbonic anhydrase it releases free carbon dioxide, which diffuses out of the blood into the lungs.
Chloride ions diffuse out of the red blood cells back into the plasma down an electrochemical gradient.
Haemoglobin in the erythrocytes also plays a role in this process.
It acts as a buffer and prevents changes in the pH by accepting free hydrogen ions in a reversible reaction to form haemoglobinic acid.
The effect of carbon dioxide
As the partial pressure of carbon dioxide rises (in other words, at higher partial pressures of CO2), haemoglobin gives up oxygen more easily.
This change is known as the Bohr effect.
The Bohr effect is important in the body because;
- in active tissues with a high partial pressure of carbon dioxide, haemoglobin gives up its oxygen more readily
- in the lungs where the proportion of carbon dioxide in the air is relatively low, oxygen binds to the haemoglobin molecules easily.